Home » Rhinoplasty Procedures » Rhinoplasty
Rhinoplasty in New Jersey
Rhinoplasty is a popular but complex nose‑reshaping surgery that requires the skilled hand of a facial plastic surgeon with extensive experience. Board‑certified facial plastic surgeon Dr. Daniel G. Becker, MD, FACS provides rhinoplasty in New Jersey, serving patients across Sewell, Voorhees, Bergen County, Essex County, Hudson County and surrounding areas.
Trust our mastery for remarkable, balanced results.
The Benefits of Rhinoplasty
Transform your life and look under the skilled hands of Dr. Becker through rhinoplasty. This surgical procedure offers more than just aesthetic refinement; it elevates your self-confidence and can significantly improve your health. Discover a multitude of advantages that pave the way for a happier, more confident you.
Boost your self-assurance and shine in every social setting. Dr. Becker’s rhinoplasty technique will help you love what you see in the mirror.
Breathe easy and live better. Rhinoplasty by Dr. Becker can optimize your airways, leading to a lifetime of healthy, unobstructed breathing.
Unveil a more balanced, beautiful you. Dr. Becker’s expertise in rhinoplasty ensures that your new nose complements your unique facial features.
What is Rhinoplasty?
Rhinoplasty, a complex nose-reshaping surgery, can significantly alter facial aesthetics and improve facial harmony. It’s particularly transformative for those dissatisfied with their nose or experiencing breathing issues.
Dr. Daniel G. Becker, MD, FACS, a board-certified facial plastic surgeon, is globally recognized for his expertise in both primary and revision rhinoplasty. Operating from two East Coast locations, he is renowned for consistently excellent outcomes.
Dr. Becker’s dedication to rhinoplasty is notable, as the procedure demands high surgical skill and precision. His career has been focused on refining the art and science of this intricate surgery, making him a sought-after expert in the field.
The Rhinoplasty Procedure Explained
More commonly known as a “nose job,” rhinoplasty is the medical term for elective nose surgery. While plastic surgeons sometimes perform primary rhinoplasty to improve breathing or structural issues, the procedure is typically performed to help patients achieve their ideal facial aesthetics and balance out the facial features. It is one of the most popular and effective plastic surgeries, yet few surgeons are truly skilled in performing this intricate cosmetic procedure.
Rhinoplasty in New Jersey can be tailored to many different needs, from cosmetic refinement to functional improvement. The Rhinoplasty Center offers a full range of nose surgery options, including:
- Primary rhinoplasty
- Revision rhinoplasty
- Ethnic rhinoplasty
- Functional rhinoplasty and septoplasty
Each procedure is customized to the patient’s anatomy and goals.
- Changing the shape of the nose and its size
- Smoothing a prominent nasal hump
- Altering the height of the bridge
- Refining the nasal tip
- Removing or altering bones and cartilage
- Adding nasal implants and grafts
- Straightening a deviated septum for better breathing
- Changing the appearance of a hooked nose
As one of the oldest facial plastic and reconstructive surgery procedures in the world, nose jobs have gone through many changes and have become a very technical procedure. Once patients have healed from their nose jobs, the results are permanent.
Rhinoplasty Before & After Photos
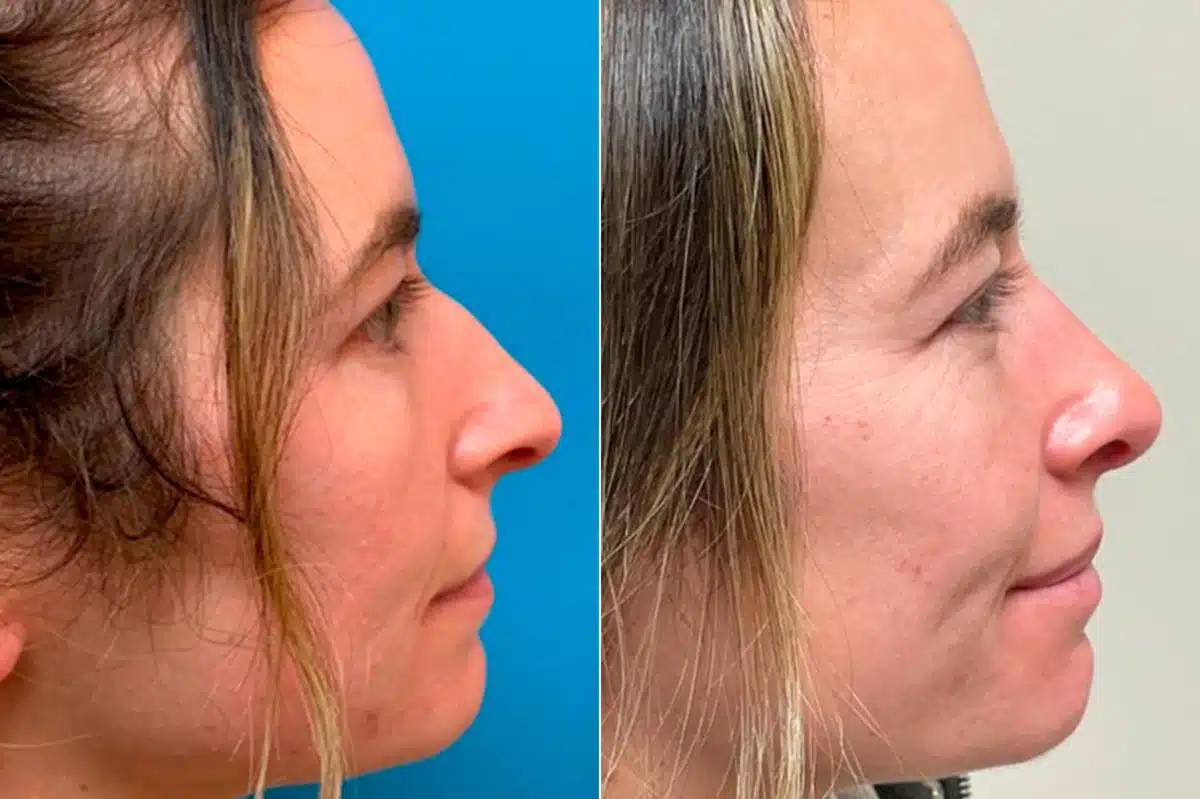
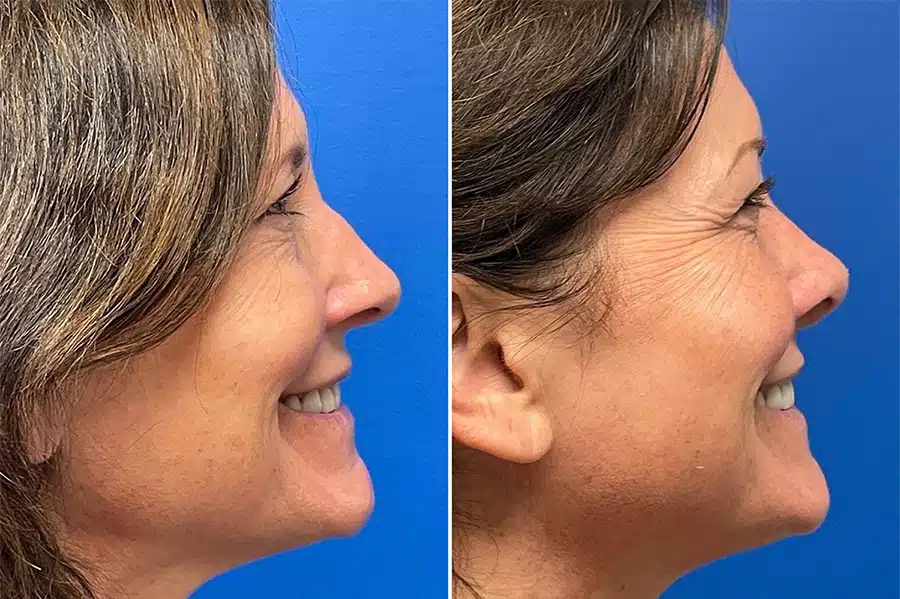
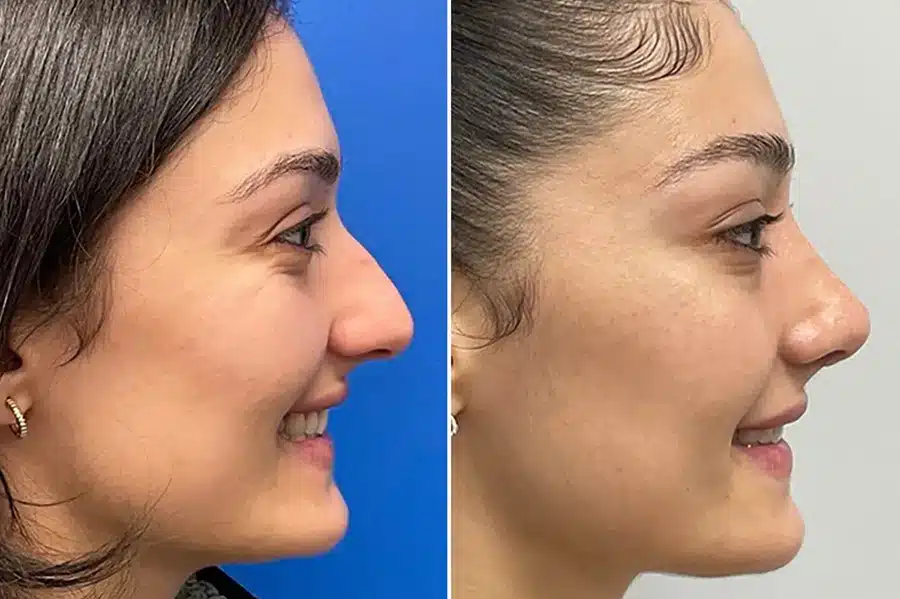
*All patients are unique and individual results may vary.
Should I Choose Primary Rhinoplasty?
Dr. Daniel Becker specializes in these surgeries, enhancing both appearance and nasal function. Rhinoplasty in New Jersey offers both cosmetic and functional benefits:
Cosmetic Reasons
- Addresses dissatisfaction with nose appearance.
- Enhances self-image in social situations and photos.
- Provides a permanent aesthetic solution beyond makeup or haircuts.
- Boosts self-esteem regardless of the nose type.
Functional and Health-Related Reasons
- Corrects issues from trauma or disease.
- Balances facial features, like a weak chin.
- Acts as an anti-aging procedure by lifting a drooping nasal tip.
Combination with Septoplasty
- Septoplasty corrects the nasal passage for better breathing.
- Insurance often covers septoplasty.
- Common to combine both procedures, especially post-trauma or disease.
Ideal Candidates for Rhinoplasty Surgery
To be considered for rhinoplasty with Dr. Daniel Becker, patients must undergo a comprehensive consultation process at his New Jersey clinic, The Rhinoplasty Center. This includes a health review, nasal examination, and possibly additional assessments. The consultation is essential for determining eligibility for this popular facial plastic surgery.
- Must be in overall good health.
- Necessary lifestyle changes for smokers or heavy drinkers.
- Control of existing medical conditions before surgery approval.
- Potential requirement of bloodwork or imaging for specific concerns.
Ensuring patient safety is a top priority for Dr. Becker and his team. During the consultation, Dr. Becker also discusses alternatives to traditional rhinoplasty, like liquid rhinoplasty. This less invasive option addresses minor issues such as nasal humps or asymmetry but requires regular maintenance, typically every few months, to sustain the results.
Real Patient Review
"Dr. Becker was absolutely amazing through the entire process of me getting my rhinoplasty"




What to Expect at a Nose Job Consultation With Dr. Daniel Becker
During the initial consultation for primary rhinoplasty with Dr. Daniel Becker, patients review their medical history and discuss any health concerns. This is also a time for patients to express their aesthetic goals, possibly with reference images of desired nose shapes. In the Rhinoplasty Consultation, Dr. Becker may use imaging to demonstrate potential post-surgery changes. He combines his expertise in facial harmony and anatomy with the patient’s preferences to customize each procedure. Dr. Becker might also recommend complementary procedures to achieve the ideal facial aesthetics.
Dr. Becker thoroughly explains the entire process, including what to expect before, during, and after surgery. He covers details like surgery location (New Jersey), anesthesia use, and specific surgical steps. Additionally, he provides crucial information for a swift recovery, including a timeline for returning to work or engaging in contact sports.
How to Prepare for a Nose Surgery
Understanding the process and following specific guidelines can greatly enhance patient comfort and facilitate healing. This guide is designed to provide essential information for patients undergoing rhinoplasty, covering critical aspects from pre-surgery preparation to post-operative care. By adhering to these recommendations, patients can confidently navigate their rhinoplasty journey with Dr. Daniel Becker and achieve the best possible results.
- Fill prescription medications for swelling, pain, and infection as directed.
- Stock up on easy‑to‑eat foods and drinks, preferably with straws.
- Prepare frozen gel packs or peas for managing swelling.
- Set up a comfortable recovery area at home with easy access to the bathroom and bed.
- Request at least one week off work, school, or normal routines, especially if you are traveling from outside New Jersey.
- Local patients can return home the same day if someone can drive them.
- Out‑of‑town patients should plan a short stay in the area for close monitoring
- The New Jersey staff or the Philadelphia ENT specialists can assist with finding suitable accommodations.
- The length of stay will be advised by Dr. Becker based on individual recovery needs and scheduled postoperative visits.
- Keep your head elevated for at least the first several days, using extra pillows.
- Avoid strenuous activity to protect the nose and reduce swelling.
- Practice good hygiene and keep the surgical area clean to lower infection risk.
- Wear button‑down shirts instead of pullovers to avoid pulling clothes over the head.
- Follow all postoperative instructions from Dr. Becker’s team carefully for a smoother recovery.
How a Surgical Rhinoplasty is Performed
Dr. Daniel Becker typically performs rhinoplasty under general anesthesia in an approved surgical facility, working with an experienced care team.
Before surgery
He meets with the patient to explain the procedure, review the planned changes, and mark the nose and face to guide the surgery. Patients are then placed in a comfortable, monitored sleep while Dr. Becker performs the procedure.
What Happens During the Procedure
Anesthesia and setup:
The surgery is performed under general anesthesia, with continuous monitoring by the medical team.
Dr. Becker reviews the surgical plan and uses facial markings to guide the precise changes to the nose.Cartilage grafts when needed:
In revision rhinoplasty, nasal reconstruction, or cases requiring augmentation, Dr. Becker often uses cartilage grafts taken from the patient’s own ear or rib.
These grafts are harvested discreetly and do not affect the appearance or function of the donor area.
In rare cases, biocompatible, animal‑derived, or cadaver‑derived materials may be used when appropriate.
Open rhinoplasty technique:
During an open rhinoplasty, Dr. Becker makes a small incision between the nostrils to access the underlying bone and cartilage.
He reshapes the nasal structure by carefully adjusting the bone and cartilage and, when necessary, adds implants or grafts.
This approach allows for precise changes to the nasal shape and nostril structure while preserving function.
Closing and stabilization:
After reshaping the nose, Dr. Becker closes the incisions with sutures.
A nasal cast is typically placed to support and maintain the new shape during early healing.
Nasal packing may be used temporarily to control bleeding and stabilize the nasal passages.
After the Surgery
Once anesthesia is reversed and the patient is awake, they are monitored until it is safe to go home or to a recovery room. Dr. Becker and his team follow a meticulous, step‑by‑step approach—from graft harvesting and bone/cartilage resizing to sutures, cast placement, and close monitoring—to ensure each stage of rhinoplasty is performed with the highest standard of medical expertise and patient safety.
Rhinoplasty Cost in New Jersey
he cost of rhinoplasty in New Jersey varies depending on the complexity of the case, whether it is primary or revision, and whether additional procedures such as septoplasty are included. On average, rhinoplasty at The Rhinoplasty Center in New Jersey falls within the range of $5,000 to $7,000, though higher‑complexity cases may be higher.
Factors that can affect rhinoplasty cost include:
Whether the procedure is primary or revision
Ethnic rhinoplasty or complex tip refinement
Combination with septoplasty or other facial procedures
Many patients qualify for financing plans through our practice, and in some cases, insurance may cover a portion of the cost when the procedure is performed for functional reasons such as breathing problems.
Rhinoplasty recovery timeline
Directly After the Rhinoplasty Procedure
Once comfortably resting, patients will often sleep much of the remainder of the day as the anesthesia wears off completely. Pain medication should be distributed by a caretaker. Patients can further control pain and swelling by lightly applying a cool compress. Any time the patient is sitting or lying down, the head should be elevated at least 45 degrees.
Before surgery, patients should request at least a week off work, school, or their normally scheduled routines.
The Week After Rhinoplasty
Patients will visit Dr. Daniel Becker’s office in the days after surgery. If nasal packing is placed, it will usually be removed within a few days. The nasal cast is typically removed one week postoperatively. Bruising is often short-lived and usually disappears around the two-week mark.
It’s essential to follow the surgeon’s instructions on cleaning the nasal area and possibly using saline sprays to keep the nasal passages moist. Most patients feel comfortable returning to work or social activities towards the end of this week, although some swelling may still be present.
The Months After Rhinoplasty and Beyond
Healing from a nose job surgery can take up to a year or longer, though much of the visible swelling and bruising will have gone down within the first few months. The nose will take on its new shape without obvious signs of surgical intervention.
Patients who are seeking a revision procedure for any reason must generally wait six months to a year after the initial procedure to allow the nose to heal completely.
Risks and Side Effects of Rhinoplasty
Cosmetic Rhinoplasty can be unpredictable for a number of reasons. The patient may have been injured while healing, developed an infection or visible scarring, or might have been dissatisfied with the results due to limitations of the anatomy. Aesthetic medicine is not a perfect science, but every precaution is taken during the consultation, surgical plan, and execution of the procedure to prevent adverse results.
Prescription medications will also help prevent infection and excessive swelling, which can impact the final look of the nose. Although rare when the procedure is performed by an experienced plastic surgeon like Dr. Daniel Becker, the following complications have been associated with this plastic surgery procedure:
| Complication | Description | Prevention and Management |
|---|---|---|
| Bleeding | Postoperative bleeding can occur, requiring careful monitoring and management. | Avoid blood-thinning medications pre-surgery, closely monitor post-surgery. |
| Infection | Risk of infection at the incision site, possibly needing antibiotic treatment. | Maintain sterile techniques during surgery, ensure proper wound care, use antibiotics if necessary. |
| Breathing Difficulties | Difficulty in breathing post-surgery due to changes in nasal structure. | Plan surgeries carefully to maintain functional airways, address any issues promptly post-surgery. |
Sometimes while healing, patients may feel concerned about the appearance of their nose. This is normal because the nose takes a long time to heal from facial plastic surgery. Nasal bones may have been broken, cartilage could have been added or removed, and significant swelling may be present. Patients are encouraged to call our New Jersey office as needed to help them feel comfortable during their recovery.
Patient-centered approach to achieving both aesthetic goals and enhanced health
Our clinic, dedicated exclusively to rhinoplasty, combines advanced surgical techniques with meticulous artistry to sculpt your ideal nose.
Reasons to Seek Rhinoplasty
Trauma to the Nasal Area (Medical Reasons)
Traumatic events like a fight, participation in group sports, and car accidents can damage the nose. A broken nose may appear crooked, have an asymmetric tip, or develop a ridge or bump. A crooked nose or a broken one may also lead to complications that include a hole in the nasal septum or the collapse of the nasal bridge which can lead to breathing problems. A rhinoplasty specialist reshapes the nose to address imperfections and breathing problems caused by the trauma
Nose Size is Unappealing
Many people are dissatisfied with the size and shape of their noses. Whether it’s perceived as too large, wide, short, or featuring a prominent hump on the bridge, rhinoplasty surgeons aim to collaborate with patients to achieve a nose they can be confident in, all while maintaining realistic expectations. The objective of a rhinoplasty, or nose job, is not to dramatically transform the nose but to enhance it in a way that harmonizes with the patient’s overall facial aesthetics. Utilizing computer imaging, surgeons facilitate discussions about surgical goals and address cosmetic concerns. It’s crucial to understand that computer imaging presents possibilities, not guarantees, serving as a tool for aligning the patient’s desires with the surgeon’s vision. This process ensures clear communication and is employed for nearly all patients before the surgery.
Tip Problems
When searching for the best rhinoplasty surgeon in New Jersey, patients should look for:
- Board certification in facial plastic or plastic surgery
- Specialization in rhinoplasty (primary and revision) rather than general plastic surgery
- Experience with complex cases, including revision and ethnic rhinoplasty
- A track record of natural‑looking, balanced results
- Transparent communication about risks, recovery, and realistic expectations
The Rhinoplasty Center in New Jersey meets these criteria, offering focused expertise in nose surgery for patients across the state.
Why Choose Plastic Surgeon Dr. Daniel Becker for a Primary Nose Surgery?
- Board Certified by the American Board of Facial Plastic and Reconstructive Surgery (ABFPRS)
- Specializes in primary and revision rhinoplasty, including functional procedures like septoplasty
- Clinical Professor of Facial Plastic Surgery (Rhinoplasty) at the University of Pennsylvania
- Founder of the Becker Rhinoplasty Center
- Author of 4 surgical textbooks and 100+ publications focused on rhinoplasty
- Director of the PENN Rhinoplasty Course since 1998, training surgeons worldwide
- National and international lecturer on advanced rhinoplasty techniques
- Consistently named a “Top Doctor” in rhinoplasty and revision rhinoplasty
- Extensive experience refining nasal shape, symmetry, and structure
- Known for conservative techniques that prioritize natural, balanced results
With decades of focused experience, Dr. Becker combines precision and artistry to deliver rhinoplasty results that enhance facial harmony while maintaining long-term nasal structure and breathing function.
The Rhinoplasty Center offers rhinoplasty in New Jersey for patients in Bergen County, Essex County, Hudson County, Union County, and surrounding areas. Dr. Daniel Becker performs nose surgery in New Jersey for both cosmetic and functional concerns, helping patients from across the state achieve balanced, natural‑looking results.
You can also explore our page about rhinoplasty near Philadelphia
Frequently Asked Questions About Cosmetic Nose Surgery
Are artificial implants used during rhinoplasty
Some plastic surgeons perform rhinoplasty procedures using biocompatible material like Gore-Tex implants, but Dr. Daniel Becker is not a proponent of this method. Gore-Tex nose jobs are more likely to become infected, and they can result in an unnatural aesthetic if the implant shifts.
How much does rhinoplasty cost?
Average rhinoplasty cost ranges between $5,000 to $7,000. The cost of rhinoplasty can vary based on the doctor’s expertise, the area of the country, and the nature of the case. Primary Rhinoplasty patients may be eligible for financing plans through Dr. Daniel Becker’s practices, or insurance may cover a portion of the cost for some subsequent or functional surgeries.
What is a tip plasty?
A nasal tip plasty is the term used for a traditional rhinoplasty surgery that focuses on improving just the tip of the nose. In some procedures, this can be performed as a liquid rhinoplasty (or non-surgical rhinoplasty), where a dermal filler is injected into the tip of the nose. However, a long-term solution is to undergo surgery. Most nasal tip plasty surgeries are faster and less invasive than full rhinoplasty.
How long does rhinoplasty surgery take?
Rhinoplasty surgery typically takes between 1.5 to 3 hours, depending on the complexity of the procedure and whether it’s a primary or revision surgery.
What is an ethnic rhinoplasty?
Non-Caucasian individuals tend to have a facial anatomy specific to their ethnicity. Dr. Daniel Becker must consider the nasal anatomy of the individual in order to achieve the patient’s desired results. He may recommend a different type of approach (Asian rhinoplasty, African American rhinoplasty). Additionally, Dr. Daniel Becker is careful to retain certain characteristics of the nose that reflect their ethnic heritage.